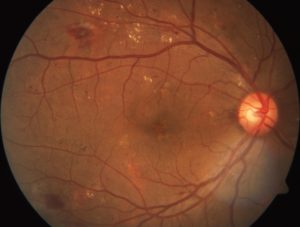
A scan of a retina showing signs of diabetic retinopathy.
A scan of a retina showing signs of diabetic retinopathy.
Living with diabetes is challenging enough on its own. Unfortunately for the 1.7 million Aussies living with the disease, it can also bring a host of potential complications.
One of those is a condition called diabetic retinopathy (DR for short, sometimes called diabetic eye disease), a serious eye condition that can cause vision loss or even blindness. It affects about one in three people with diabetes.
Fortunately, you can prevent DR from progressing if you find and treat it early enough.
But that’s where it gets tricky.
The doctor will see you now… the specialist, a bit later
Screening for DR is complex, and currently only ophthalmologists and optometrists can screen for it. A person with diabetes visits their GP as part of routine management for their condition, and that’s when their GP might recommend they get tested for DR. The GP then refers them to see a specialist for that test, and they go on a waiting list.
They might wait up to three months, because specialists are by definition specialists (funny, that), so they’re in high demand. Then the person is screened. If they don’t have signs of the condition: excellent! If they do, and need treatment, they might have to wait again depending on severity.
As you can see, early detection and long wait times don’t go hand-in-hand.
But with the latest work from our researchers in Western Australia, we’re trying to make the process easier for everyone – and help people get diagnosed and treated sooner.
Getting smart: the AI software that taught itself
Over in Perth, our researchers have just finished trialling a world-first, artificial intelligence-driven technology that enables GPs to scan people for diabetic retinopathy themselves.
Affectionately dubbed ‘Dr Grader’, the software learned by analysing ophthalmologists’ grading data, improving its ability to detect various signs of the condition.
It was recently trialled at the GP Superclinic @ Midland Railway Workshops. GPs scanned 187 diabetic patients’ retinas, and the high resolution images were then analysed by both our grading software and a real-life ophthalmologist for signs of the condition.
Our research director, Professor Yogi Kanagasingam, said the results speak for themselves: the technology detected signs of DR as effectively as the ophthalmologist.
“If this technology is rolled out, GPs could scan patients for the condition and its severity, then refer them to an ophthalmologist for further investigation and treatment based on the severity of their symptoms,” Yogi said.
“This way we could reduce unnecessary referrals, potentially reduce waiting periods for patients, and help ophthalmologists focus on patients who need treatment and surgery.”
The software’s licenced by TeleMedC, who plan to roll it out to 20 GP clinics in WA over the next few months, with a view to eventually expanding across Australia.


31st October 2017 at 8:40 pm
Informative article. Thanks for sharing
8th October 2017 at 8:12 am
Very informative will certainly look into this
5th October 2017 at 11:03 pm
It is usefulness!
21st September 2017 at 2:07 pm
Excellent work.
20th September 2017 at 10:16 am
Interesting and informative