The latest results by Aussie scientists might in the future make it easier for doctors to predict a person’s risk of developing Alzheimer’s disease, paving the way for new treatments.
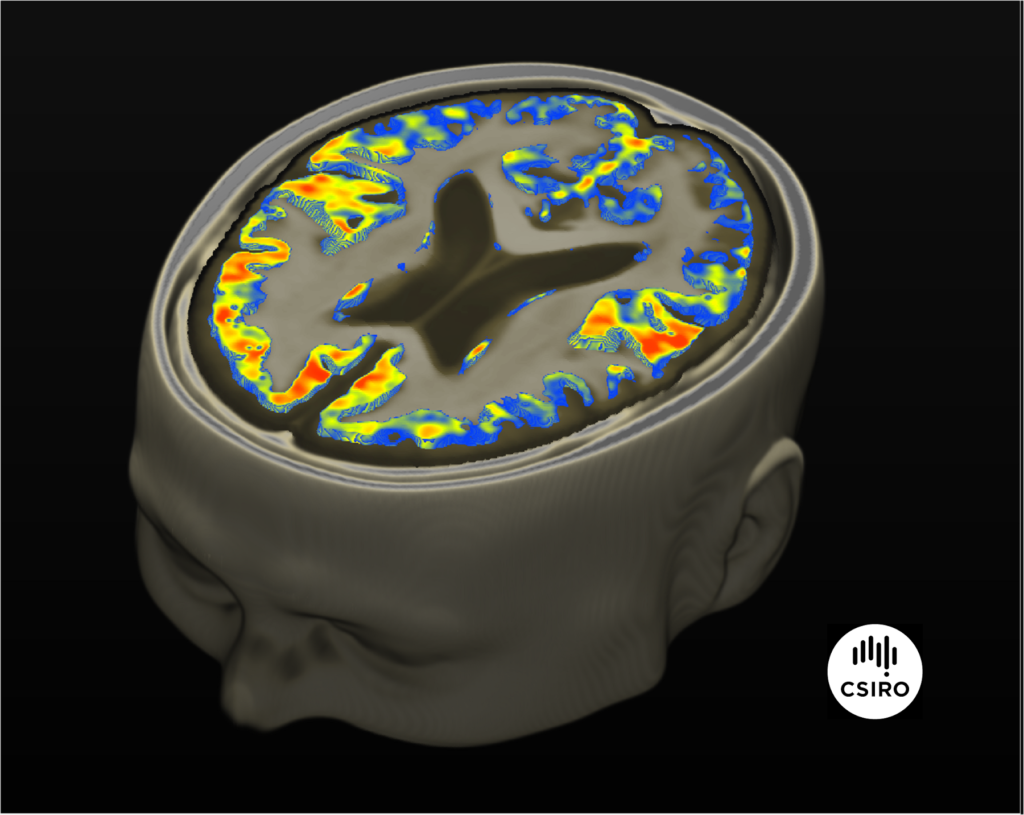
The overall differences in terms of the iron-sensitive biomarker between people with high and low level of Amyloid protein in the Frontal, Temporal and Hipocampal regions (the hotter the colour, the higher the differences )
The overall differences in terms of the iron-sensitive biomarker between people with high and low level of Amyloid protein in the frontal, temporal and hippocampal regions (the hotter the colour, the higher the differences).
Alzheimer’s disease can be devastating. It accounts for more than half of all cases of dementia, which is the second leading cause of death in Australia, and can take a real toll on families.
But the latest results by Aussie scientists might in the future make it easier for doctors to predict a person’s risk of developing Alzheimer’s disease, and pave the way to develop new treatments. And the technology is pretty space-age: essentially a sophisticated metal detector for your brain.
Iron: the metallic x-factor
Now, scientists have long believed that the slow build-up of amyloid (fragments of a protein) in the brain triggers a cascade of events that leads to people developing Alzheimer’s Disease. About a third of people in their 70s have a lot of amyloid in their brain, but, some don’t lose cognitive abilities like short-term memory, executive function and language ability as quickly as others.
Some other factor had to be involved. It turns out that something else may be iron.
Teaming up with the Florey Institute of Neuroscience, the Australian Imaging Biomarkers and Lifestyle (AIBL) study, and the CRC for Mental Health, our scientists studied 117 older Australians who were either normal or in the process of coming down with Alzheimer’s.
They found that the rapid deterioration of cognitive function (basically, how well your brain works) was linked to iron levels in the brain. Their paper’s just been published in the journal called, fittingly, Brain.
The scientists measured amyloid and iron levels in the brains of the 117 participants, and followed them in the AIBL study, performing cognitive function testing every 18 months for the next 6 years. The researchers found amyloid in the brain only mattered for cognitive deterioration when iron levels in the brain were high.
The higher the brain iron concentration, the faster brain function decline in people who had amyloid in their brain, at any stage of the disease- even before the onset of symptoms.
Iron needle in a brain haystack
Don’t go reaching for Great Uncle Albert’s metal detector just yet. The levels of iron we’re talking about require equipment a lot more sophisticated.
MRI technology – which uses magnetic fields and radiowaves to make images of your brain – has been around for a while, but recent improvements have allowed subtle changes in iron to be measured
Using these improvements, the biomedical informatics team has been able to map out and pinpoint likely iron deposits in the brain. This could be used to better estimate the risk that someone is likely to develop Alzheimer’s disease as well as the timing of the onset of deterioration.
Trialling potential new treatment
So, if Alzheimer’s progression is faster when you have more iron in your brain alongside amyloid, it makes sense to investigate if reducing the iron slows the disease down. This is a promising new avenue for drug treatments, particularly for people with Alzheimer’s who are at risk of declining cognition.
To test the theory, Florey scientists plan to use an existing drug, deferiprone, to ‘mop-up’ excess iron in the brain and see if it slows down the disease’s progression. This will soon be trialled in Australia’s major cities.
If you’re 65+ and noticed your memory’s declining, or if you’re newly diagnosed with dementia, you can register your interest to be involved in the study by emailing 3D@florey.edu.au. Eligible participants will be contacted when the study opens for enrolment later this year (2017).


6th September 2017 at 10:04 pm
There seem to be so many routes one can take to Dementia. It seems Amyloid Protein build-up alone could just be a symptom of one of these many and varied routes. Congratulations to your researchers in identifying another possible element in this complex and baffling process.
10th August 2017 at 4:38 pm
How is the iron content of water likely to affect this finding?
31st July 2017 at 3:25 pm
Can the amyloid buildup in the brain be due to not getting enough exercise. The question i would then like to ask… is partaking in exercise use more iron. Argentina for example is a greater meat consumption nation than australia. What are the rates of dementia in Argentina? If they are comparable then iron might indeed have a part to play.
29th July 2017 at 1:50 pm
Presumably a normal intake of iron is not the problem, rather it is its concentration in the brain, which deferiprone will mop up there but not elsewhere?
26th July 2017 at 4:36 pm
Very interesting- does that mean if you have a lower iron intake, eg vegetarian you have a better chance of not getting it even if your family is heavily linked with it? A Gousmett
28th July 2017 at 4:43 pm
No. Diet and iron supplements would not affect iron levels in the brain, according to a related news article: http://www.abc.net.au/science/articles/2015/05/20/4238548.htm.